Informational nature
The information presented in this text is scientific and educational in nature. It is intended to explain the molecular, cellular, and systemic mechanisms of glucagon action within a physiological context.
This text does not address dosing regimens, clinical indications, or therapeutic applications. The information is based on peer-reviewed scientific literature and is intended to support a general understanding of biological mechanisms.
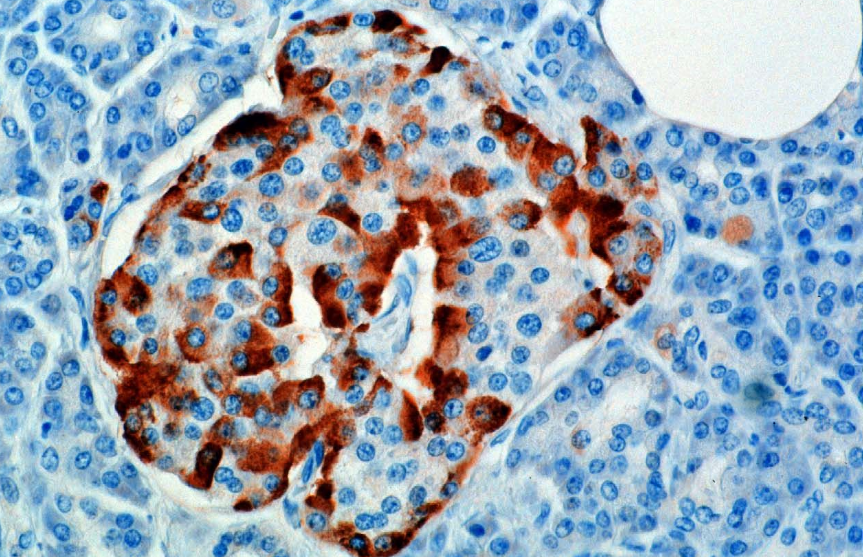
The human body maintains blood glucose levels within a narrow range. This balance is regulated by multiple hormones acting in a coordinated manner, among which glucagon plays a central role as a counter-regulatory hormone to insulin.
Glucagon is involved in energy mobilization processes, particularly during fasting or under conditions of reduced blood glucose levels [1,2].
Keywords: glucagon; glucagon receptor; G protein–coupled receptors; cAMP; glycogenolysis; gluconeogenesis; energy homeostasis; pancreas; α-cells
Historical background
Glucagon was identified in the early 20th century through studies investigating the effects of pancreatic extracts on blood glucose levels [1].
Subsequent research demonstrated that this hormone is produced by pancreatic islet α-cells and serves as a key regulator of glucose homeostasis [2].
Advances in molecular biology enabled the identification of the glucagon receptor and its signaling pathways, thereby elucidating a complex network of hormonal regulation [3].
Molecular structure and receptor
Glucagon is a 29–amino acid peptide hormone derived from the precursor proglucagon [1,2].
It exerts its effects via the glucagon receptor (GCGR), a member of the class B G protein–coupled receptor (GPCR) family [3].
Receptor activation results in increased intracellular cAMP levels and activation of PKA-mediated downstream signaling pathways [3,4].
GCGR is predominantly expressed in the liver but is also present in other tissues involved in metabolic regulation [2,3].
Key physiological mechanisms
Glycogenolysis
When blood glucose levels decline, glucagon stimulates the breakdown of hepatic glycogen into glucose.
This process, known as glycogenolysis, represents a primary mechanism for rapid energy mobilization [1,2].Gluconeogenesis
Glucagon also promotes gluconeogenesis—the synthesis of glucose from non-carbohydrate substrates in the liver [2,4].
This mechanism becomes particularly important during prolonged fasting.Lipid metabolism aspects
In experimental models, glucagon signaling has been associated with fatty acid oxidation and ketone body production in the liver [2,5].
The physiological relevance of these processes depends on overall metabolic conditions and concurrent hormonal signals.Interaction with insulin
Glucagon and insulin act in a coordinated manner:
- insulin promotes energy storage,
- glucagon promotes energy mobilization.
This counter-regulatory balance maintains systemic glucose homeostasis [1,2].
Methodological context
Glucagon biology is studied across multiple levels:
- the molecular level,
- cell culture models,
- animal models,
- human physiological observations [1–6].
Interpretation of results depends on:
- study design,
- model selection,
- metabolic state,
- statistical methodology.
Data derived from experimental models may not fully recapitulate the complexity of human physiology; therefore, their interpretation requires careful contextualization.
Research directions
Current research focuses on:
- structural and functional properties of the glucagon receptor [3],
- interactions between signaling pathways and other hormonal systems [2,4],
- tissue-specific receptor expression,
- the role of glucagon in systemic energy homeostasis [5,6].
These research directions aim to advance understanding of the mechanisms underlying metabolic homeostasis.
Discussion
Glucagon constitutes a central component of systemic energy regulation. Its effects are context-dependent, influenced by nutritional status, physical activity, and interactions with other hormonal signals.
Signaling via cAMP and PKA pathways represents only one element of a broader regulatory network. Biological systems are inherently dynamic: hormone concentrations fluctuate, receptor sensitivity may vary, and signaling pathways exhibit extensive cross-talk [2–4].
Accordingly, analysis of a single hormone does not fully capture systemic responses. Glucagon function should therefore be interpreted within the framework of an integrated endocrine regulatory system.
Conclusions
- Glucagon is a 29–amino acid peptide hormone synthesized by pancreatic α-cells [1,2].
- Its receptor signaling is mediated via cAMP-dependent mechanisms, particularly prominent in hepatic tissues [3,4].
- Glucagon is involved in glycogenolysis, gluconeogenesis, and broader processes of systemic energy mobilization [1,2,5].
- Its effects are context-dependent and modulated by interactions with other hormonal systems.
References
[1] Müller TD, et al. Glucagon: Physiology and Pathophysiology. Physiological Reviews. 2017.
https://doi.org/10.1152/physrev.00013.2016
[2] Holst JJ, et al. Glucagon and amino acid metabolism. Endocrine Reviews. 2018.
https://doi.org/10.1210/er.2018-00069
[3] Mayo KE, et al. International Union of Pharmacology. The Glucagon Receptor Family. Pharmacological Reviews. 2003.
https://pubmed.ncbi.nlm.nih.gov/12615996/
[4] Jiang G, Zhang BB. Glucagon and regulation of glucose metabolism. American Journal of Physiology-Endocrinology and Metabolism. 2003.
https://doi.org/10.1152/ajpendo.00492.2002
[5] Campbell JE, Drucker DJ. Islet α cells and glucagon—critical regulators of energy homeostasis. Nature Reviews Endocrinology. 2015.
https://doi.org/10.1038/nrendo.2015.51
[6] Unger RH, Cherrington AD. Glucagonocentric restructuring of diabetes. Cell. 2012.
https://doi.org/10.1016/j.cell.2012.02.031


